A first person surgical perspective.
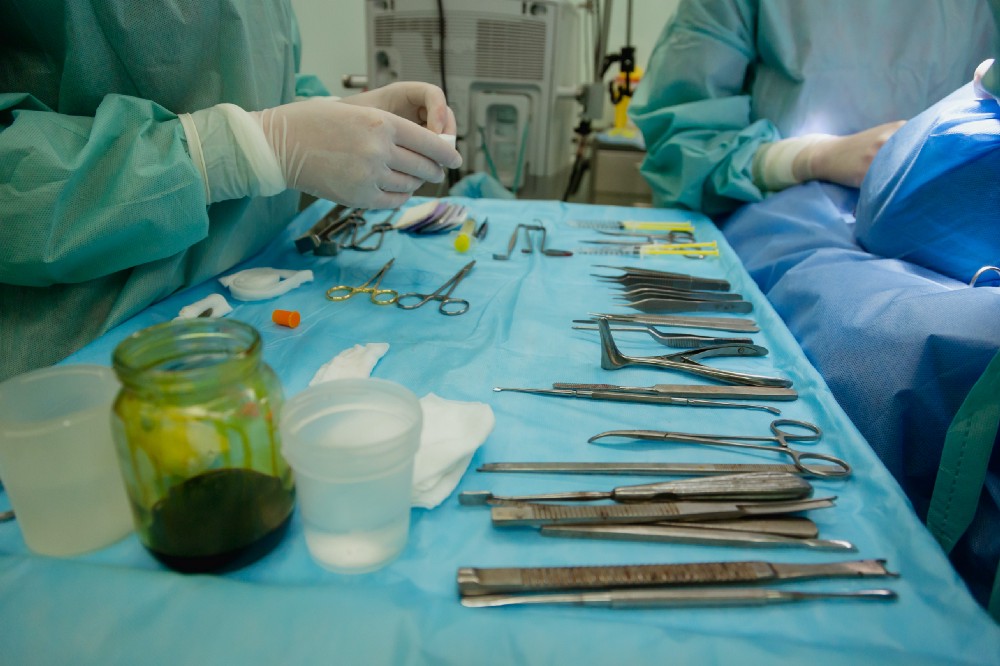
I stare down at my gloved hands. They appear nearly translucent as the moisture remaining from my surgical scrub adheres my skin to the latex. The bright white light from above contrasts with the relative dull of the surgery suite. The surgical lights bathe everything in front of me in an artificial glow. Shimmering skin visible underneath the surgical drape. The instruments on the tray next to me glimmering with anticipation. The sharp glint catching my eye from the scissors, the forceps, and everything else. All neatly arranged; if only for a moment.
I look down at the task before me. Everything is ready for the next step, the first in what will likely be a long, taxing procedure. The whine of the blood pressure cuff as it begins to fill meshes with the rhythmic beep of the ECG as my patient lies stable, deep under anesthesia. My task today is to remove a gigantic tumor. A common task for us in the veterinary world. This mass popped up about a month ago per my client, but over the last few days began to grow rapidly. We scheduled this surgery as an emergency to attempt to solve it before it became a more serious problem. My grumbling stomach reminds me of the lunch break I was supposed to be having.
The scalpel blade clicks into place on its handle, and I position my hand to make the cut. Beginning the procedure, the blade separates flesh from flesh. Elliptically, I slice around the mass of interest. The freshly scrubbed skin separates neatly underneath the scalpel like a peach beneath a paring knife. Below the skin surface, the light reflects even stronger. The subcutaneous tissues are brighter than the skin. The white sheen of fat and fascia (the thin sheath that covers muscle) is the next layer to go. Falling like corn beneath a scythe as my scalpel continues its cleanly destructive path. This massive tumor has been allowed to grow for too long, and I’m here to stop it.
The superficial tissues gone; I can begin to see the full extent of my task. The heat underneath the surgical lights is intense, the first fifteen minutes of surgery have flown by. “How’s he doing?” I ask of my technician monitoring anesthesia. “He’s doing okay, heart rate is stable, but the blood pressure is down a little.” “Knock the anesthetic gas down, we’re going to be here for a while,” I instruct focusing back on the task in front of me. The deeper layers require a bit more tact than the superficial ones. I can’t just slice through them with the scalpel and hope for the best. This is where the major blood vessels and nerves live.
Using my scissors, I bluntly push through the necessary tissues beginning, bit by bit, to free this tumor from the bonds beneath. In some areas, the normal tissue is beyond recognition and I am forced to try to guess at where this invasion ends and normal begins.
With each cut, I run the risk of hitting a major artery or vein. When I identify a blood vessel, I encircle it with suture and tie it off, or ligate it. This prevents it from bleeding, and it will atrophy (wither away) once the mass is removed. I arrive at the area of the body where I know a large blood vessel to be. I switch from my scissors to hemostatic forceps to gently push the tissues out of the way. The forceps are much blunter than scissors, so they come with lower risk. My hands steady as I press small pieces of muscle and surrounding fat out of the way. I’m searching methodically for the large vessel so I can ligate it before it can bleed. I nudge a piece of tissue out of the way only to be greeted by a fountain of blood. A bright red stream from the surgical site dousing the drape in crimson.
“Shit,” I mutter to myself, startling my technician a little. I reach quickly for my surgical pack, grabbing another pair of hemostatic forceps, and am able to clamp the bleeding culprit off. This stems the tide for now, giving me a chance to finish it once and for all. I encircle the vessel in suture, cinching down around it. For good measure, I drive my needle through the vessel and tie it off again slightly above the previous tie. This ensures it won’t be creating problems for me again. I remove my surgical clamp to ensure the bleeding is truly stopped and get back to work.
An hour has zipped by, and the mass is about 95% removed. The tissues underneath glistening as I approach the final cut. This time, I see it before disaster strikes. The last portion of tissue that I must remove is pulsing, as if alive on its own. A large artery lives inside this tissue. The pulsation matches nicely with the constant beep of the ECG monitor. Using the smallest hemostats that I have, I gently remove the tissue that surrounds this monstrous blood vessel to isolate it. The vessel was likely the supply of nutrients for the mass, allowing it to get so large so quickly. I watch my suture glide into a constrictive knot around the artery. Satisfied to see the pulsing occurring only on one side of my suture now; I cut the final clump of tissue. This giant tumor’s last desperate hold on my patient. It is free. I place the block of tissue into a jar of formalin so that the laboratory can tell me what it is. I have my suspicions already.
Now that the mass is removed, the hard part begins. I stare into the maw that I’ve created. The elliptical incision is imperative to allowing a large portion of tissue to be removed while still retaining the ability to close it afterwards. Staring at the task in front of me, the telltale feeling of unease creeps its way into my gut. “Why do cancers have to make things so damn difficult.” It is one thing to remove a tumor from the body, it is an entirely different task to close it appropriately afterwards.
I equip a relatively large suture to my needle drivers and begin the process. An hour at least, I expect. My patient lies blissfully unaware of the battle that I am waging on their behalf. First, any muscles that were cut need to be reattached to facilitate their rapid healing and alleviate some of the post surgical pain. The edges severed in the process are slowly reattached. One stitch at a time. Next, the subcutaneous tissues need to be closed. These contain fat, fascia, and some other connective tissues. Special suture ties are used for this process to alleviate tension over the canyon that I’ve created. Slowly, the incision comes together, piece by piece, stitch by stitch. The chasm slowly becomes a gorge and then a ditch. Each suture that I place narrowing the gap by a slight margin. Finally, all areas of the subcutaneous layer have been secured. Now, the skin must be apposed. This final step will complete my task. I used to count each suture as I placed them, now I just place them without regard to the total number. Neatly the skin comes together kissing at the edges as if trying to spark life where life has just been removed. The scar will be impressive, but we have beaten this tumor for now.
I tie the final knot and slowly step back from the table. The sickening white lights still glare overhead, the temperature beneath them easily five degrees warmer than the rest of the room. The task is complete. The anesthetic gas is clicked into the off position. Only oxygen flows into my patient’s lungs now. They’ll be awake soon. The rest is up to them, I’ve done what I can for now. I remove my surgical gloves and place them on the pack to be cleaned. The surgical drape is removed from the patient and placed into its own bin for disposal. Pain medication is injected around the incision to provide some relief. Finally, my surgical gown is removed. The relief is immediate, almost like removing a glove from my entire body. The airflow returns and I can feel my body start to cool. The excitement and the focus of the procedure slowly dissipating and allowing normal sensation to return. I wash my hands, watching the beads of water slowly roll off, whisking the bubbles of soap from them in the process. Surgery is finished, it’s finally time for lunch.



Wow, great description. It sounds intense and your writing brought me in for the whole procedure. I hope the patient fully recovered and that the tumor was benign.
LikeLiked by 1 person